Scoliosis, a complex spinal condition that affects millions of people worldwide, can be quite challenging to navigate. That’s why we've put together this comprehensive guide to help you better understand your scoliosis disability. We’ll cover the various types of scoliosis, including idiopathic, degenerative, neuromuscular, and congenital. Our goal is to provide you with valuable insights into the symptoms of scoliosis, empowering you to take control of your spinal health. So, let's dive in and unravel the complexities of scoliosis together!
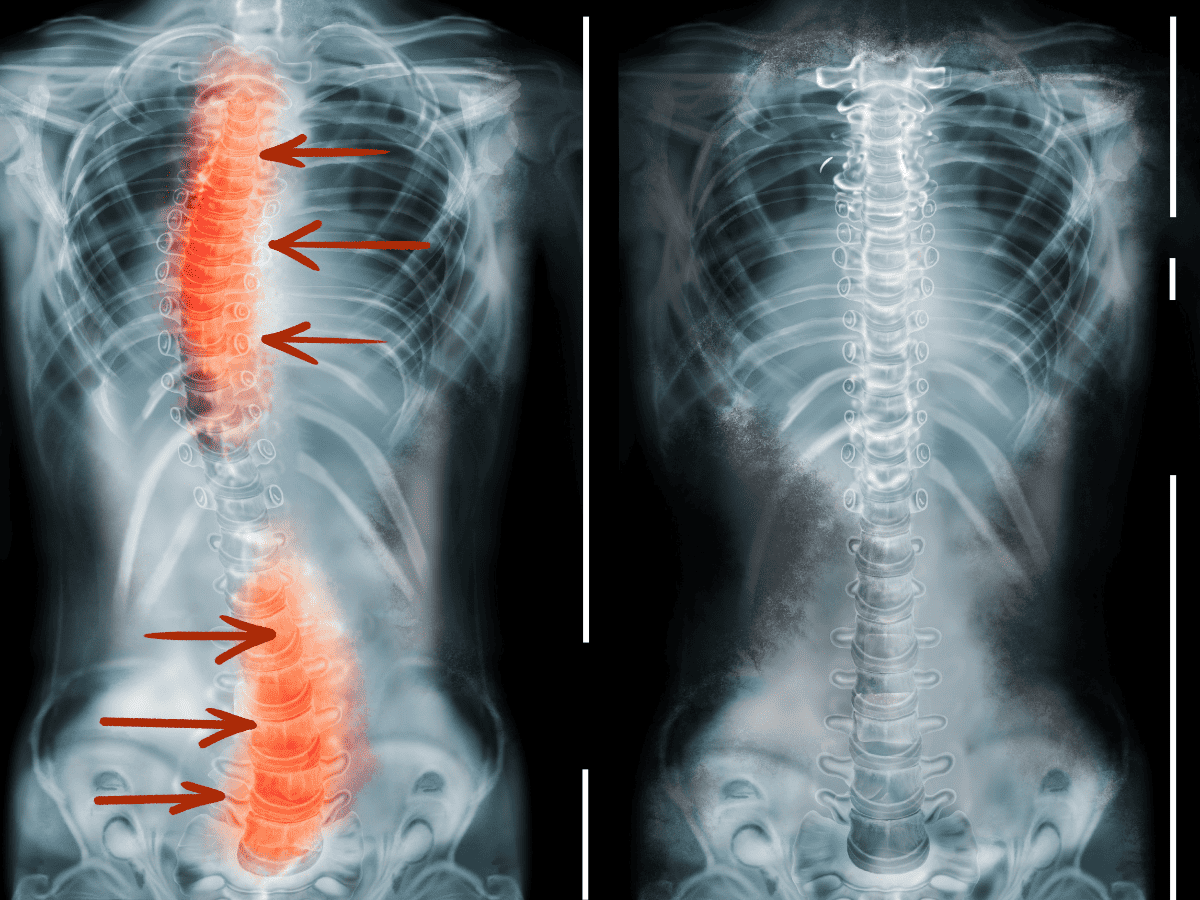
What is scoliosis? It’s a condition where the spine curves unnaturally to the side, resulting in an abnormal posture for patients. Mild scoliosis can develop subtly, often going unnoticed by those affected. Mild scoliosis may sometimes not cause significant discomfort or require treatment. However, severe cases can lead to stress and strain on internal organs, making it essential to address the issue. One contributing factor to scoliosis development is spina bifida, a birth defect that affects the spine. Spina bifida can sometimes cause scoliosis in children, adding to the importance of early detection and intervention.
This is the most common type of scoliosis, accounting for around 80% of cases. Adolescent idiopathic scoliosis is quite common, as this condition typically affects age groups including infants and juveniles. The reason it's called idiopathic scoliosis is because the exact cause remains unknown, although researchers suspect that genetic factors such as family history may play a significant role. Diagnosing idiopathic scoliosis often involves a thorough physical examination, X-rays, and, in some cases, additional imaging tests.
This will depend on many factors including the patient's age, ranging from simple observation and monitoring to physical therapy, bracing, or even surgery in more severe cases. Early intervention is key in managing idiopathic scoliosis, as it can help prevent the progression of the spinal curve and minimize its impact on the individual's overall health and well-being.
Degenerative scoliosis, also known as adult-onset scoliosis, is a less common form of the condition compared to idiopathic scoliosis. It primarily affects adults over the age of 40 and is closely linked to the natural aging process, which can cause spinal wear and tear. As individuals advance in age, the risk of developing this type of scoliosis increases, with factors such as the degeneration of intervertebral discs, arthritis, and osteoporosis potentially contributing to its onset.
Typically, we will start with conservative approaches, including pain management and physical therapy. However, in severe cases or when conservative treatments prove ineffective, a surgical treatment like spinal fusion or decompression may be recommended to alleviate pain and improve spinal stability.
This is a type of scoliosis that arises due to underlying neurological conditions, such as cerebral palsy, muscular dystrophy, or spinal cord injuries. These conditions can result in muscle imbalances and weakness, which may contribute to developing abnormal spinal curvature. Although less prevalent than idiopathic scoliosis, neuromuscular scoliosis can significantly impact an individual's quality of life. Diagnosis typically involves a comprehensive evaluation of the patient's medical history and imaging tests like X-rays or MRI scans.
Treatment options vary depending on the severity of the curvature and the specific neurological condition involved. In some cases, physical therapy and bracing may be sufficient to manage the condition. However, more severe cases may require surgical intervention to stabilize the spine and alleviate associated symptoms. It's essential for individuals with this type of scoliosis to work closely with their healthcare team to develop a tailored treatment plan addressing their unique needs.
Congenital scoliosis is a rare form of the condition that occurs when the spine develops abnormally during fetal development. This type of scoliosis is present at birth and is caused by malformations in the vertebrae, such as hemivertebrae (half-formed vertebrae) or fused vertebrae. These structural abnormalities can lead to an uneven distribution of weight along the spine, resulting in abnormal curvature. Diagnosing congenital scoliosis typically involves a detailed review of the patient's medical history, a thorough physical examination, and imaging tests like X-rays or CT scans to assess the extent of the spinal anomalies.
Treatment options for congenital scoliosis depend on the severity of the curvature, the specific vertebral malformations, and the patient's age and overall health. In some cases, conservative treatments like bracing or observation may be recommended. However, more severe scoliosis cases or those with progressive spinal curves may require surgical intervention to correct the spinal deformity and prevent further complications. At Long Island Brain and Spine, our team of specialists collaborates closely with patients and their families to develop a personalized treatment plan that best addresses the unique challenges posed by congenital scoliosis.
Prevention and management strategies play a crucial role in maintaining spinal health and addressing the challenges posed by scoliosis. Regular checkups and monitoring are essential for early detection and timely intervention, which can help minimize the progression of spinal curvature and its impact on an individual's overall well-being. Physical therapy and exercise contribute significantly to strengthening the muscles that support the spine, improving posture, and promoting flexibility. Depending on the severity of the condition, bracing or surgical options such as spinal fusion surgery may be recommended as part of a comprehensive treatment plan. In addition to medical interventions, coping strategies, and support resources are invaluable for individuals with scoliosis, as they can provide emotional and practical assistance throughout the journey towards better spinal health. By embracing a proactive approach to prevention and management, those affected by scoliosis can improve their quality of life and maintain a healthy, active lifestyle.
Cerebral palsy is a group of neurological disorders that affect muscle coordination and body movement, often caused by damage to the brain during pregnancy, birth, or early childhood. The curvature of the spine is often associated with it, which is why scoliosis is seen as a secondary condition. Scoliosis can develop in individuals with cerebral palsy due to muscle imbalances, weakness, or spasticity, which can pull the spine out of alignment.
Scoliosis is a complex spinal condition with various types, including idiopathic, degenerative, neuromuscular, and congenital scoliosis. Each type has unique characteristics, causes, and treatment options, highlighting the importance of accurate diagnosis and tailored treatment plans. At Long Island Brain and Spine, our team of skilled professionals is dedicated to providing comprehensive care for individuals affected by scoliosis. By staying informed about the latest advancements in scoliosis research and treatment, we can offer our patients state-of-the-art care and support throughout their journey to better spinal health. Whether you or a loved one is navigating the challenges of scoliosis, you can trust the compassionate and knowledgeable specialists at Long Island Brain and Spine to guide you every step of the way.
1. What is scoliosis? Scoliosis is a medical condition where the spine curves unnaturally to the side, resulting in an abnormal posture for patients. The severity of scoliosis can vary, with some cases being mild and others causing significant discomfort or complications.
2. What causes scoliosis? The exact cause of scoliosis is often unknown, but it can be linked to genetic factors, neuromuscular conditions like cerebral palsy, or birth defects such as spina bifida. In some cases, scoliosis can develop as a result of injury, infection, or tumor growth.
3. What are the symptoms of scoliosis? Symptoms of scoliosis can include uneven shoulders, hips, and waist, back pain, difficulty breathing, and fatigue. However, mild scoliosis may not cause noticeable symptoms or discomfort.
4. How is scoliosis diagnosed? Scoliosis is typically diagnosed through a physical examination and imaging tests, such as X-rays, MRI, or CT scans. These tests help physicians assess the severity of the spinal curvature and determine the best course of treatment.
5. Can scoliosis be treated? Yes, scoliosis can be treated through various methods, depending on the severity of the condition. Treatment options include observation, bracing, physical therapy, and surgery. The goal of treatment is to prevent the progression of the curve, alleviate pain, and improve overall quality of life.
6. Is scoliosis a lifelong condition? Mild scoliosis may not require ongoing treatment, but more severe cases may need long-term management. With proper care and treatment, many people with scoliosis can lead active, healthy lives.
7. How does Long Island Brain and Spine approach scoliosis treatment? At Long Island Brain and Spine, our team of skilled physicians is dedicated to providing comprehensive care for patients with scoliosis and related conditions. We utilize advanced diagnostic tools, conservative treatments, and surgical interventions to help patients achieve improved mobility, reduced pain, and enhanced quality of life.